The course is often similar: at the beginning, the symptoms of Covid-19 are often not very pronounced: cold symptoms, cough, aching limbs, loss of smell and fatigue. After some time, everything seems to be overcome.
But the old strength does not return. Everything is difficult - even thinking. Drowsiness, difficulty concentrating, difficulty finding words, shortness of breath, palpitations and sometimes feelings of panic.
What is it? What should be done?
Long Covid
Definition and frequency
Long Covid is a significantly debilitating symptomatology secondary to Covid-19 disease. The main symptoms are fatigue, arthralgias and myalgias, anxiety, depression, cognitive impairment and sleep disturbances.
There are varying data on the frequency, ranging from 15% to over 70% % of primary sufferers of Covid-19 . In hospitalized patients, 72% of sufferers suffered from Long-Covid in a German study. However, symptomatology also occurs after milder, non-hospitalized forms of the disease.
Causes and risk factors
There is currently no clarity about the causes. A multifactorial genesis is assumed. Risk factors are mainly female gender, physical pre-existing conditions, lung diseases such as asthma, overweight and psychiatric pre-existing conditions with depression, anxiety disorders or traumatic pre-existing conditions.
Frequency
There are varying study results on the incidence, ranging from 10% to more than 70% % of primary covid-19 sufferers. In hospitalized patients, 72% of those with covid suffered from long covid in a German study. Similar findings apply to ventilated patients. However, symptomatology also occurs after milder, non-hospitalized forms of the disease. Here, the incidence is lower but the study situation is still unclear.
In the extensive Gutenberg study, one in three did not regain their original performance capacity. Those knowingly infected were slightly more likely to have limitations (about 30%) compared with those unknowingly infected (22.4%). However, a similar number of individuals (22%) complained of post-Covid-like symptomatology, although no infection was detectable.
The number of symptoms was highest in the first 3 months after infection. By postinfection month 6, the decline was marked. Then, in the further course of time, the number of symptoms decreased much more slowly.
Using a conservative estimate, it can be assumed that at least 10% of infected persons develop longer-lasting symptoms in the sense of a post-covid.
Long Covid and the respiration
Dysfunctional breathing
In addition to exhaustion, persistent dyspnea is at the center of the symptomatology for those affected. Up to 80% of hospitalized patients report this. This occurs as exertional dyspnea after minor, sometimes minimal physical exertion, or as feelings of anxiety, the feeling of not being able to breathe, or as thoracic pressure sensations.
Although changes in lung function can be detected in 22-56% even after 6 months, the extent of the changes found does not explain the severity of the impairment in many cases.
Therefore, as early as 2020, dysfunctional breathing was assumed to be a possible (partial) cause of the complaints.
In one study, 20.9% were found to have an abnormal score with respect to the most commonly used test to detect dysfunctional breathing (Nijmegen questionnaire). In another study, the proportion of patients with hyperventilation was as high as 50%.
In a separate online study of 147 patients who reported having experienced Covid-19 disease, the average response was 21 out of 62 points, close to the threshold for dysfunctional breathing of 22 points.
Several variables may be altered in dysfunctional breathing: such as respiratory rate, depth of breath, or increased mouth breathing. However, the long-term consequence is a biochemical shift associated with high oxygen saturation, decreased CO2, slightly elevated pH, and slightly decreased bicarbonate. Electrolyte shifts may also occur as a result of alkalosis.
Because decreased CO2 leads to cerebral underperfusion, this mechanism may explain a greater proportion of the complaints (fatigue, cognitive impairment, feeling of not getting enough oxygen). Decreased cerebral blood flow with lowered CO2, particularly during standing, was found in a smaller study of long-covid syndrome.
Based on our own experience with 132 long covid patients, we were able to measure either a decreased pCO2 in blood gas analysis and/or respiratory gas analysis in the majority of affected patients, or there was clear evidence of an accompanying hyperventilation problem in the online history collection.
The abnormalities often do not occur at rest ( sitting/lying) but only when standing, walking, or with mild hyperventilation. This observation has also been reported by other authors. There is overlap with postural tachycardia and CFS (chronic fatigue syndrome).
Other cardiological symptoms (palpitations, dysrhythmias) could be explained by alkalosis leading to a change in electrolytes (decrease in ionized calcium, potassium, magnesium).
Thus, it stands to reason that dysfunctional breathing is (partly) responsible for central aspects of the long covid syndrome.
Consequences of dysfunctional breathing
Online Breathing Training
(copy 2)
Eine dysfunktionelle Atmung findet sich nicht nur bei Post-Covid, POTS oder CFS. In den vergangenen 10 Jahren konnten wir bei einer Vielzahl von somatoformen und funktionellen Störungen Hinweise auf z.T. ausgeprägte Veränderungen finden. Besonders eng war der Zuammenhang bei Panikattacken, funktionellem Schwindel (PPPD), Derealisation, Reizdarm und somatoformen Schmerzstörungen (z.B. Fibromyalgie, Vulvodynie).
Ausgehend von den Arbeiten von Meuret et al. zur dysfunktionalen Atmung bei Panik und Asthma haben wir daher in den vergangenen Jahren ein Therapiekonzept entwickelt, um die veränderten Atemgasparameter gezielt zu verändern. Im Mittelpunkt steht dabei ein Biofeedbackverfahren, bei dem über eine Atemgasbestimmung der erniedrigte CO2-Spiegel im Blut gemessen und dann in sehr kleinen Schritten normalisiert wird.
Für dieses Verfahren (Capnometer-assistiertes Atemtraining) liegen Arbeiten vor, die eine Evidenz bei der Therapie von Asthma bronchiale, Panikattacken und anderen körperbezogenen Ängsten und posttraumatischen Belastungsstörungen nachweisen.
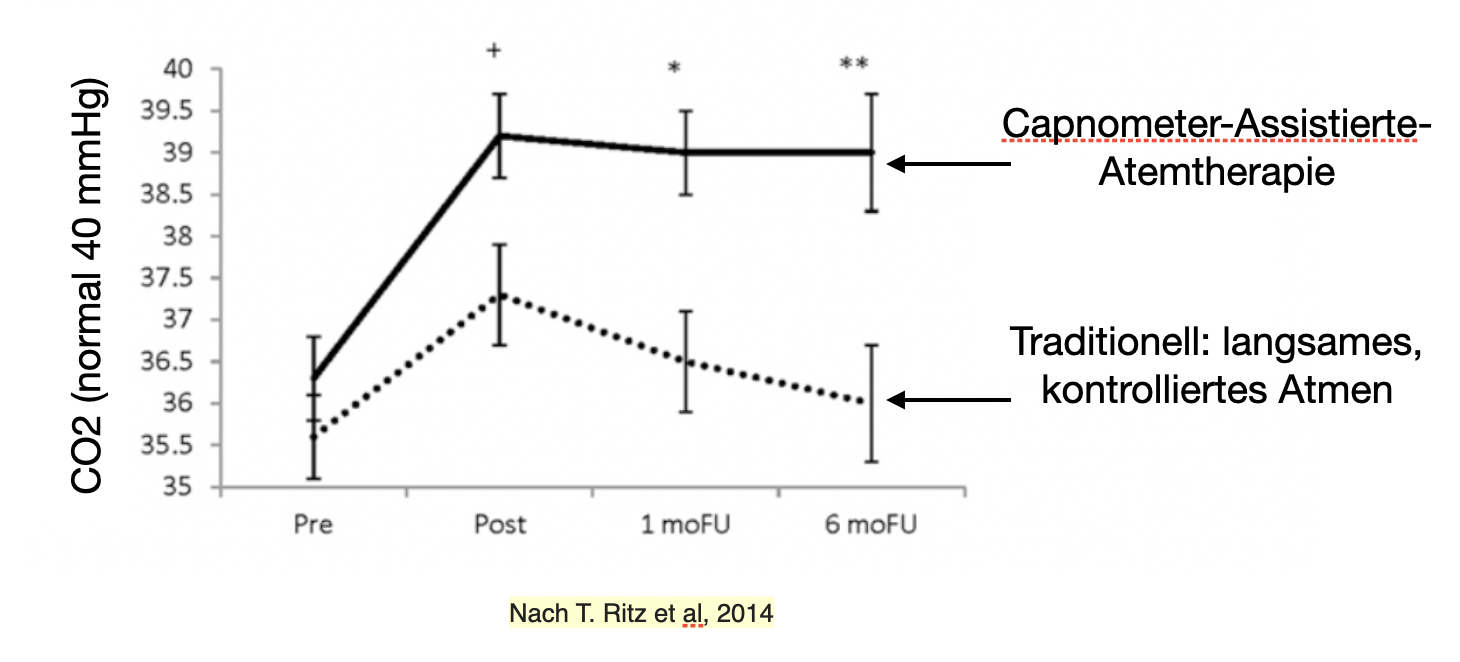
Im Vergleich zu traditionellen Atemtechniken (z.B. nach Buteyko) zeigte das Capnometer-assistierte Atemtraining deutliche bessere Effekte. Der Anstieg des pCO2 war höher und die Wirkung blieb über 6 Monate erhalten, während bei der traditionellen Atemtherapie der Anstieg geringer war und keine Konstanz über die Zeit aufwies.
(copy 3)
Online-Atemtraining
Während wir bei den Behandlungen vor Ort, diese Atemtraing in eine multimodale Therapie integrieren, haben wir parallel ein Online-Training entwickelt, um Patienten behandeln zu können, die aus verschiedenen Gründen nicht anreisen können. Vor allem der geringe Aufwand, die Möglichkeit zuhause und ggf. auch vor/nach der Arbeit zu trainieren und die Eignung des Verfahrens auch für sehr geschwächte Personen wurde von den Betroffenen geschätzt. Nicht zuletzt sind die Kosten erheblich geringer.
Verfahren
Die Indikation und diagnostische Einschätzung erfolgte in einem etwa 30minütigen online Arztgespräch.
Falls sich die Patienten für das Verfahren entschieden, wurde Ihnen ein Gerät zur Bestimmung des CO2-Gehalts der Atemluft (Kapnograph, Masimo-Corporation) für durchschnittlich 30 Tage überlassen.
Parallel erhielten die Patienten einen Link für die Registrierung bei einer Online-Atem-App.
Danach erfolgte eine 30minütige Online Einführung in das Gerät und die Nutzung der App durch speziell ausgebildete Physiotherapeut/innen. Bei Bedarf war es den Patienten möglich weitere Online Termine sowohl bei den Physiotherapeuten oder Arzt in Anspruch zu nehmen. Die Häufigkeit dieser Physiotherapie-Atem-Sitzungen schwankten von 2-10 Sitzungen nach individuellem Bedarf.
Im Mittelpunkt des Trainings steht die online-App, die den Umgang und das Biofeedbackverfahren mit dem Kapnographen vermittelt, sowie mehrere weitere Trainingsmodule umfasst. Damit soll auch online ein mutlimodale Ansatz verfolgt werden. Wesentliche Elemente sind
- Atemtechniken
- Entspannungsverfahren
- Physiotherapeutische Übungen
- Umfangreiche Informationselemente zu verschiedenen Krankheiten jeweils in Form von Videos.
Die Betroffenen wurden angehalten mehrfach pro Tag zu üben. Bei einer Online-Befragung berichteten die Nutzer, sie würden mehrfach pro Tag zwischen 5-15 Minuten mit der App arbeiten. Die gesamte Trainingsdauer schwankte zwischen 15 Minuten und etwa zwei Stunden pro Tag.
Bei einer Umfrage zu einer frühen Version berichteten 86% der Teilnehmer, App und Kapnograph sei hilfreich oder sehr hilfreich für sie und ihre Beschwerden gewesen. Eine aktuelle Untersuchung ist in Vorbereitung.
(copy 5)
Notwendigkeit leicht verfügbarer Therapieverfahren
In Deutschland waren bis Frühjahr 22 mehr als 20 Millionenen Menschen an Covid-19 erkrankt. Selbst wenn von der konservativen Schätzung von 10% Post-Covid-Fällen ausgegangen wird, bedeuten 2 Millionen Post-Covid-Patienten eine kaum zu bewältigende Aufgabe. Die BAR-Frankfurt zählt ca. 35.000 Betten in Kliniken mit Post-Covid-Programm. Das stellt bereits zwei Drittel der Gesamtkapazität aller Reha-Kliniken dar.
Allerdings gibt es aktuell kein allgemein anerkanntes Therapieverfahren bei Post-Covid. Die Effektivität der derzeit angebotenen Programme ist daher zumindest mit Unsicherheit behaftet.
Hinzu kommt: Selbst wenn sämtliche verfügbaren Therapieplätze mit Post-Covid-Patienten belegt würde und nur jeder Zweite der Post-Covid-Patienten einen Reha-Platz erhält, würde es fast zwei Jahre dauern, bis der letzte der bis heute Erkrankten einen Therapieplatz erhalten hat.
Doch in der Zwischenzeit dürften viele weitere Millionen der bis heute nicht Erkrankten (> 50 Millionen) einen Therapieplatz benötigen.
Derzeitiger Stand
Aktuell haben wir verschieden Apps entwickelt, die im Rahmen eines Post-Covid-Online-Programm eingesetzt werden können.
Im Zentrum steht die Atem-App, die ein spezifisches Atemtraining ermöglicht. Diese App enthält daneben umfangreiche Entspannungs- und Meditationstechniken, Achtsamkeitsübungen, Anleitung zur progressiven Muskelrelaxation und autogenem Training.
Es gibt weiterhin eine App für das Traininig des Kreislaufes, sofern Symptome einer posturalen Tachykardie besehen.
Ein umfrangreiches Bewegungs- und stufenweises Bewegungsprogramm für Patienten mit und ohne körperliche Einschränkungen, das für die Rheumliga Baden-Württemberg entwickelt wurde.
Beispielfilm
Nächste Entwicklungsstufe
Die nächsten Entwicklungsstufen sehen folgendes vor:
Stufenweises Kursprogramm, in dem die Nutzer von in jeder Stufe mehrere Elemente kennenlernen und durch Übungen geführt werden
- Informationen zum Krankheitsbild
- Verhaltensempfehlungen (z.B. Pacing)
- Atemübungen mit ohne Kapnometer
- Entspannungsverfahren
- Meditative Verfahren
- Dehnübungen
- Angepasst Bewegungsübungen
In den folgende Stufe(n) gelangen die Teilnehmer, nachdem sie eine Reihe von Fragen beantwortet haben.
Nach jeder Stufe wird ein einfaches Assessment der Beschwerden durchgeführt (z.B. visuelle Analogskalen, Verständnisfragen). Der Erfolg spiegelt sich in einem Dashboard wieder.

